There was a time -- not very long ago -- when Bangladesh could speak with confidence about its success in controlling measles. The country had been internationally recognized for its immunization programs and achievements.
It had significantly expanded vaccination coverage, dramatically reduced child mortality, and established itself as a successful model of low-cost, community-based public health. Measles, once a deadly childhood disease, seemed to be on the verge of elimination.
That confidence is now becoming fragile.
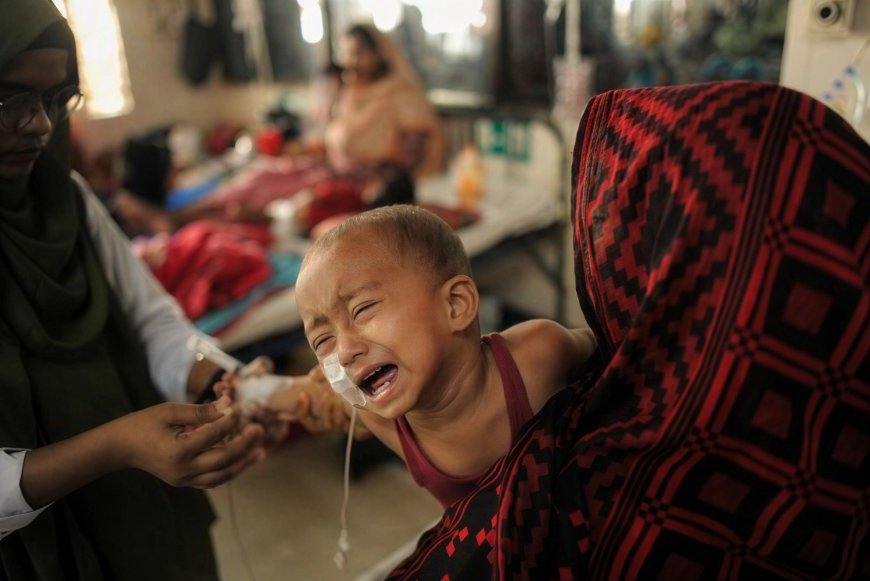
Recent reports of rising measles infections among children, along with nearly 200 preventable child deaths, are not merely a public health issue; they are a serious warning. This is not just about a virus -- it reflects something deeper: The stark reality and fractures within Bangladesh’s health governance system.
The Spread of a Preventable Tragedy
Measles is not a mysterious disease. It is one of the most contagious viruses in the world, yet also one of the most preventable. Two doses of the vaccine provide near-complete protection. Still, it is resurging in Bangladesh, and hundreds of children are dying.
The problem is not the absence of vaccines -- it is that vaccines are not reaching everyone. According to joint estimates by UNICEF, WHO, and GAVI (Global Alliance for Vaccines and Immunization), around 500,000 children in Bangladesh are still not fully immunized, even though national coverage hovers around 81–82%.
This gap is not abstract. It directly creates a large pool of vulnerable children -- those most at risk of infection. Health experts have already warned of a “surge wave” of measles among children in 2026, increasing the risk of complications such as pneumonia and death. In today’s world, every child death from measles represents a systemic failure -- because it should not happen.
The Illusion of High Coverage
On paper, Bangladesh appears to be doing well. Official figures indicate about 96% coverage for the first dose and over 90% for the second.
These numbers are impressive -- but they conceal a dangerous reality. The truth is that coverage is not uniform.
Vaccination rates are significantly lower in urban slums, remote rural areas, and among displaced populations -- especially within the Rohingya community. UNICEF has repeatedly highlighted that these immunization gaps are concentrated among hard-to-reach and marginalized groups.
As a result, herd immunity breaks down in specific pockets. And measles does not require national failure to spread -- local weaknesses in health governance are enough.
Where Governance Breaks Down
It is easy to view measles outbreaks as technical problems -- issues of vaccine supply, cold chain, or logistics. But the real issue runs deeper: It is fundamentally a crisis of health governance. Health governance determines how decisions are made, how systems are coordinated, and how accountability is ensured. And it is here that Bangladesh faces significant challenges.
First, coordination gaps persist. The health system -- comprising government programs, NGOs, and international partners -- has expanded, but also become fragmented. Responsibilities overlap, while gaps remain, particularly in last-mile service delivery.
Second, surveillance remains reactive. In many cases, outbreaks are detected only after they spread. Real-time, community-level monitoring is still weak.
Third, inequality is structural. Policies are national, but implementation is local. Without targeted strategies, marginalized populations are left behind.
Fourth, accountability is limited. High coverage statistics mask local failures. Without independent verification and community oversight, it is difficult to ensure that every child is reached.
In short, health governance works -- until it doesn’t.
A Warning from Global Trends
Bangladesh’s experience is not isolated. The World Health Organization has warned that when immunization systems weaken, measles is often the first disease to return -- acting as an early warning signal. Recent global data show a resurgence of measles in multiple regions due to declining coverage and delayed responses. The lesson is clear: Public health progress is not permanent -- it can erode, even reverse.
Beyond Vaccines: The Trust Deficit
Another subtle but critical challenge is trust.
During COVID-19, misinformation and vaccine hesitancy increased globally. Fortunately, Bangladesh remained relatively protected from this trend. Parents are generally aware and willing to vaccinate their children -- especially in urban areas. Yet even small levels of hesitancy can weaken herd immunity.
It is in this context that the failure of the interim government led by Dr. Muhammad Yunus becomes evident. By appointing an extremely weak, inexperienced, and ineffective adviser based on personal familiarity and retaining her despite repeated failures -- the leadership caused significant damage to the health system.
During that adviser’s tenure, the national measles vaccination campaign scheduled for late 2024 was cancelled. Even more concerning, procurement contracts for vaccines were cancelled without securing alternative sources.
We must recognize that immunization is not just a public health intervention -- it is also a social contract. Parents must trust that vaccines are available, safe, and reliably delivered and that the health system stands with them. This trust cannot be built through campaigns alone. It requires sustained community engagement, local leadership, and transparent communication.
What Must Change
The loss of hundreds of children cannot be addressed through emergency vaccination drives alone. Structural reforms are essential:
Focus on equity, not just coverage : Identify and reach “zero-dose” children, rather than relying on national averages.
Strengthen routine immunization: Campaigns are important -- but they cannot replace regular services.
Invest in real-time data systems: Digital tracking can enable faster, targeted responses.
Empower frontline workers: Community health workers need training, incentives, and support.
Ensure accountability: Independent audits, community monitoring, and transparency must be strengthened.
Rebuild public trust: Go beyond awareness campaigns -- listen to communities.
A Moral Test of Governance
At its core, this measles outbreak is not just a health sector issue -- it is a test of governance. Immunization is one of the most cost-effective public health interventions. The knowledge exists. The tools are available. The infrastructure is largely in place. Yet children are dying.
Because measles is not inevitable -- but governance failure is.
An independent and impartial investigation into the causes of the current outbreak is essential. It must examine policy decisions, administrative failures, and any negligence or corruption. Those responsible must be held accountable. At the same time, the voices of families who have lost their children must be heard. That is a moral obligation of the state.
A Warning Signal
Time has not yet run out for Bangladesh. The situation has not yet escalated into a full-blown crisis; but it is a clear warning. Many countries have ignored such warnings and paid a far greater price later. Bangladesh’s past success shows what is possible. The present reality reminds us of the risks.
If geographic, social, and institutional gaps can be addressed, measles elimination is still achievable. But if failures in health governance persist, measles will not be the last disease to return. And the cost will not be measured in statistics -- but in the lives of children who should never have been lost.
Dr. Khalilur Rahman is a former Ambassador and Secretary to the Government of Bangladesh, and a Senior Public Health Policy Adviser at the World Health Organization (WHO).